Last Resort: The hidden truth about how dying people end their own lives in the UK

Warning
This report contains accounts of dying people ending their own lives.
A list of organisations that can provide support and information around terminal illnesses, end-of-life care, bereavement, suicidal thoughts and mental health can be found here.



Dad could have had a longer life and a kinder, safer death.
Are they going to prosecute me?
Am I going to go to prison?
What’s going to happen?
She decided that she wasn’t going to let cancer do its worst.
She would construct a way to escape.
Three failures of the law

In 2017, we published The True Cost: How the UK outsources death to Dignitas.

In 2019, we published The Inescapable Truth: How seventeen people a day will suffer as they die.

This final report - Last Resort - examines the third way in which the current law fails dying people.
It reveals the stories of those who feel they have no other option but to take matters into their own hands.
It explores their motivations and lays bare the repercussions for those who are left behind.
It looks at the ways in which the police struggle to enforce the law and examines how we might quantify how many dying people in the UK take their own lives each year.


Language

Language around the assisted dying debate is contested.
In 2016, the term assisted dying was added to the Oxford English Dictionary.
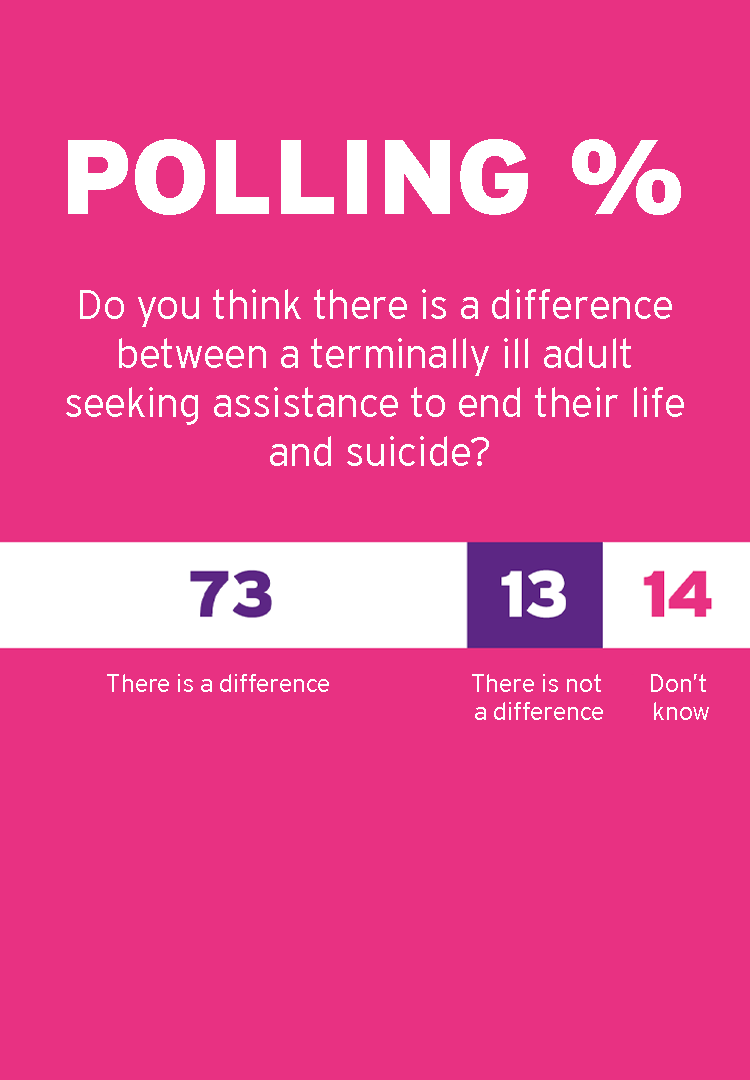
However, most campaign groups opposed to assisted dying legislation instead favour the term ‘assisted suicide’, arguing that there is no difference between a dying person who chooses to control the manner and timing of an imminent death and someone who dies by suicide.

It is widely accepted that the term suicide carries social stigma and the idea that a person ‘commits’ suicide is an outdated reference to when – prior to the 1961 Suicide Act – suicide was a crime.
Even in the circumstances explored in this report, where people have ended their own lives, interviewees were keen to highlight the importance of distinguishing their loved ones’ actions from suicide.
Dignity in Dying rejects the term ‘assisted suicide’ and this report does not refer to dying people controlling the manner and timing of their deaths as having died from suicide.
The public agrees.


She never used the word suicide,
just always said,
‘Don’t worry
about me, I’ll sort myself out.’

Other means

Research has uncovered cases of dying people in the UK who have ended their own lives from a range of highly distressing and violent means.
I have had to think through other options just in case I am unable to get to Switzerland. I have worked out where I could end my life. I have thought about getting drugs.
I am not suicidal.
If I could choose life over my inevitable fate I would, but I can’t.
The uncertainty of various methods people used created significant anxiety, as did the knowledge for some people of what their dying loved one was planning.

She started to stockpile any prescription that she had. I had to go to the chemist and collect her medicines for her, she was too ill to do that herself.
In all honesty I was quite frightened but I was just was focusing on taking care of her.
The dark web consists of a hidden network of websites. It allows people to access and use the internet anonymously and while some people use it for legitimate means it has become renowned for illegal activity, including being a place where marketplaces for drugs are hosted.

Scams and fraud on the dark web have been uncovered, which no doubt creates anxiety for dying people who are trying to purchase substances for a specific use at a specific time in a clandestine manner in order to protect their families. This route also exacerbates inequalities given the resources and knowledge needed to navigate the process.
A couple of policemen knocked at the door, and I thought, ‘Well what are you here for?’ having contacted him half an hour or so before.
They said, ‘We’re very sorry but your son’s been killed.’ One of the side roads to the hospital has a junction with a major road.
A witness saw him run into the second lane, where he was hit by an HGV.


Attempts

In our interviews we did not encounter any examples where somebody who attempted to end their life and survived did not try again. The experiences featured in this report all involve people who died at their first attempt or people who tried multiple times to end their own lives.
This contributes to an understanding of the differences between dying people ending their own lives and non-dying people who die by suicide.
There were three attempts. Who knows what didn’t work and why and what kind of pain and damage that did to his body. Surely we would wish for it to be done safely, around your loved ones and not in such a lonely, lonely and difficult way?
The presence of a chronic illness is already considered a risk factor for repeated suicide attempts. In 2007, a report on the National Suicide Prevention Strategy for England acknowledged the presence of ‘painful illnesses’ as a factor that increased the likelihood of someone taking their own life.

Adam explained how his mum tried to end her own life by overdose on a number of occasions.
I went up to see her and she was just lying in bed fast asleep and I woke her up and she was very confused, she said, ‘Why am I here?’
I said, ‘What do you mean?’
And she goes ‘I shouldn’t be here.’ She told me to…she told me to leave her alone. She had taken a lot of her medicine and I got there too late.
Adam’s mum did not end her own life. She died in a hospice. There was a haemorrhage in her throat and she choked on her own blood.

The way she went out was bloody awful, it really was. You sit in a room as a husk just slowly ebbing away and that’s not really fair in my opinion because that’s not how she would have wanted to go.


Crime scenes

Throughout the UK the police are expected to attend all incidents of sudden or unexpected deaths that occur outside of a medical setting.

In 2012 the Association of Chief Police Officers, now the National Police Chiefs’ Council (NPCC), issued guidelines on dealing with cases of assisting or encouraging suicide. It is clear from our interviews that some police officers were uncomfortable investigating possible cases of assistance in line with the NPCC guidance, though many interviewees were sympathetic to the plight of the police in these circumstances.
I turned up and she was lying upstairs. I asked the police if I could just go up and give her a kiss which I did and then they turned round and said, ‘You know we’re going to have to investigate this.’

For others the police appeared to have acted in a way that lacked sensitivity. There is dramatic inconsistency in the way these deaths are investigated.
When they took our phones they said they were asking permission to download photos, internet history, messaging and call history and I said, ‘Well what happens if we say no?’ And they said, ‘Then we will have to wonder why you’re saying no to something like that.’


Grief


There is much to differentiate the deaths of the people featured in this report from cases of suicide, yet one aspect where similarities remain is the immediate impact on those who are bereaved. This might be due to the fact that some interviewees discovered their loved one’s body, were denied an opportunity to have an open conversation with their loved one about their feelings and intentions or live with regret at the manner in which their loved one died.

These effects were compounded for some interviewees in this report because they also witnessed their loved ones suffering prior to their death and/or feared the potential legal implications following their loved one’s death, for them and for other people they knew, including the possibility of prosecution and imprisonment.
These negative outcomes contrast with what we know about bereavement in countries where some form of assistance to die is legal. A study of family caregivers of people who had accessed assisted dying in Canada found they overwhelmingly viewed the quality of their loved one’s death more favourably than the one they anticipated by ‘natural causes’, namely because of the prevention of unnecessary suffering.

Interviewees described many symptoms of complex grief, a term that is used to describe grief that is distinct from bereavement-related loss and is a predictor of long-term functional impairments.
A couple of months after she passed away I had had enough and I tried to end my life. I don’t remember too much about it. I just couldn’t understand, if that makes sense? I didn’t want to carry on. If she’d gone off how she wanted and I knew that, I would have been happier I think, you know?
It still makes me angry because I know that the sense of touch is the last sense to go and it’s still upsetting for me that I was not able to provide that sort of last sense.
We didn’t know how the DPP guidelines would be applied, so we didn’t take any risk in the situation. Then the whole thing unfolded with the police which made it impossible for me to have that emotional support from my family on the first day.
While research on the impact of witnessing a stranger end their life is scarce, qualitative studies have found negative effects, including post-traumatic stress disorder, flashbacks and physical reactions such as sweating, nausea and trouble breathing when they are reminded of the event. Support resources for third party witnesses of suicide describe it as a life-changing event with shock, nightmares, difficulty sleeping, flashbacks, substance abuse, irritability, guilt and anxiety as common reactions.
When they rang the police up, they sent out a first responder. Because it was in a fairly small village, they haven’t got an ambulance guy in a rapid response vehicle.
The first responder is a volunteer in the community; he was a teacher at the local high school.
He had to cut him down.



Assisted dying

Over 200 million people in the world have access to some form of assisted dying. Interviewees for this report told us why their loved ones would have had better, less traumatic death if this was an option in the UK.

The difference with assisted dying would have been night and day. There would have been much more control, there’s nothing wrong with wanting a little control of one’s life. It would have enabled her to have lived the last part of her life with optimism, with positivity.
She would have enjoyed the sunrises and the sunsets a lot more knowing that she was going to have a good death.
There would have been somebody there to be with him, to hold his hand, people that loved him.

It would have made an enormous difference. He wouldn’t have had to panic for six months whilst he got everything sorted out.
I wouldn’t have spent three years thinking, ‘What if it goes wrong?’


Summary and recommendations

This report has found catastrophic failings in the UK’s blanket prohibition on assisted dying.
A lack of meaningful choice is driving dying people towards deaths that are often violent, dangerous and lonely. The difficulty of having honest conversations with healthcare professionals, as well as unequal knowledge and unequal access to expertise of how to die, creates disparities and some people are denied the ability to have the death that they want. The law fails to protect dying people.
The uncertainty that surrounds the planning process and the clandestine nature with which plans have to be put in place creates anxiety for dying people. It also affects family members and friends, who not only have to cope with worries about how their loved one will die, but they can also experience trauma after witnessing their loved one end their own life and must then also confront the problems that occur in the immediate aftermath, including being the subject of police investigations.
All of this is compounded by knowledge that dying people in other jurisdictions around the world have access to assisted dying, which offers an open and legal process for exercising the choices they wish to make.
While the Office for National Statistics is now investigating this problem, an historic failure in data collection has the problems that dying people face. Based on all the evidence available to us, we now estimate that between 300 and 650 dying people end their own lives in the UK every year, with a further 3,000 to 6,500 making an attempt on their own life.




Every year in the UK...
The law must change to allow terminally ill, mentally competent adults the option of an assisted death, subject to robust, upfront safeguards
A change in the law would reduce anxiety, inequalities and unnecessary suffering amongst dying people in the UK. Crucially, it would make society safer, replacing the chaos of the status quo with a law that is open and transparent and has meaningful upfront protections, both for those who would want to explore the option of an assisted death and those who would not. This is in stark contrast t the current law, where investigations tend to take place after someone has died, if they happen at all. Law change would provide an opportunity for robust data collection and regulation, providing a much more accurate picture of the end-of-life choices dying people in the UK wish to exercise.

There must be recognition that assisted dying and suicide are distinct concepts
People who are terminally ill and approaching the end of their lives simply want to control the way they die. Presenting this as ‘suicide’ is misleading. It does not reflect the academic literature or the views of dying people and their families and leads to a lack of clarity in the assisted dying debate. In line with guidelines from the Samaritans, the phrase ‘commit suicide’ is inappropriate in any circumstance. As this report shows, many terminally ill people feel driven to end their lives in lonely and violent ways. An assisted dying law would protect these people from those kinds of deaths.

Society must know the true numbers of dying people who end their own lives in the UK
The Office for National Statistics (ONS) is currently researching the rates of deaths recorded as suicides amongst dying people. The ONS should routinely collect and present this data to Parliaments in the UK to inform debates about assisted dying. Those with relevant expertise should work together to explore how further data could be collected. The Coroner’s Society of England and Wales should consider ways that it can contribute its expertise and knowledge to societal debates.

Dying people should be able to have open and honest conversations with others about their wish for an assisted death
Those who want to control the manner and timing of their deaths should not have to manage that wish alone out of fear of implicating their loved ones or healthcare professionals in a crime. Organisations that provide care and support to dying should assess their policies on assisted dying to ensure they are creating space for their members, staff and service users to have conversations about the subject. They should ensure they are pro-actively promoting a culture of openness and respect for diversity of views around choice at the end of life.
Police forces should review their procedures for responding to deaths where a dying person has ended their own life
Police officers should not be asked to instigate investigations into breaches of the 1961 Suicide Act without sufficient training and support. Grieving relatives should not be subjected to unnecessarily intrusive and insensitive police investigations immediately following the death of their loved one. Police forces should review their existing procedures and learn from previous investigations they have conducted. Organisations responsible for other first responders should also ensure that people have the support they need to respond to and deal with these cases.



We can wish it were not true.
We can choose to ignore it.
We can turn to flawed reasoning to justify it.
But when the history books scrutinise how we confronted the question of assisted dying we will no longer be able to claim ignorance of the horrors inflicted by its prohibition.
If you think you oppose assisted dying, all we ask is that you look at this evidence, and then think again.
A more detailed version of this report is available here:
We are building a network of people willing to share their experience to help us strengthen the case for law change.
If you have a story to share, please get in touch.
Resources

The following organisations can provide information and support around terminal illness, end-of-life care and bereavement.
Compassion in Dying
0800 999 2434
www.compassionindying.org.uk
Cruse Bereavement Care
0808 808 1677
www.cruse.org.uk
Cruse Bereavement Care Scotland
0845 600 2227
www.crusescotland.org.uk
Hospice UK
020 7520 8200
www.hospiceuk.org
Macmillan Cancer Support
0808 808 00 00
www.macmillan.org.uk
Marie Curie
0800 090 2309
www.mariecurie.org.uk
Motor Neurone Disease Association
01604 250505
www.mndassociation.org
MND Scotland
0141 332 3903
www.mndscotland.org.uk
The following organisations can provide information and support to anyone struggling to cope with suicidal thoughts and mental health.
Samaritans (UK)
116 123
www.samaritans.org
Lifeline (Northern Ireland)
0808 808 8000
www.lifelinehelpline.info
Breathing Space (Scotland)
0800 83 85 87
www.breathingspace.scot
Hafal (Wales)
01792 816 600
www.hafal.org
Mind
0300 123 3393
www.mind.org.uk
Mind Wise (Northern Ireland)
www.mindwisenv.org
Rethink Mental Illness
0808 801 0525
www.rethink.org
Sane
0300 304 7000
www.sane.org.uk
Change Mental Health
0808 8010 515
www.changemh.org/
